
Eczema in children is one of the most common skin conditions a parent will ever encounter. According to the American Academy of Pediatrics, eczema in children, also known as atopic dermatitis, affects between 20% and 25% of babies and young children worldwide, making it the most prevalent chronic skin condition in childhood. Despite how common it is, however, eczema can be deeply distressing for both the child who experiences it and the parents who are trying to help.
The itching, redness, and sleepless nights that come with eczema in children can feel overwhelming, especially when you are unsure what is causing the flare-ups or how to bring your child relief. The good news, however, is that eczema in children is very well understood medically, and with the right knowledge and consistent care, most children experience significant improvement, and many outgrow the condition entirely as they get older.
In this guide written specifically for parents, we cover everything you need to know: what eczema in children looks like at different ages, what triggers it, and, most importantly, the practical soothing strategies you can use every day at home. If your child’s eczema is severe or persistent, our specialist dermatology team is here to provide expert, personalised care.
What Is Eczema in Children?
Eczema in children, most commonly atopic dermatitis, is a chronic inflammatory skin condition caused by a combination of genetic predisposition, a compromised skin barrier, immune system dysfunction, and environmental triggers. In simple terms, children with eczema have skin that is less able to retain moisture and protect itself from external irritants and allergens. As a result, the skin becomes dry, inflamed, and intensely itchy.
Importantly, eczema in children is not caused by poor hygiene, and it is not contagious. A child cannot pass eczema to another child through touch or contact. Furthermore, eczema often runs in families; if one or both parents have eczema, asthma, or hay fever (a trio collectively known as the atopic triad), their children are significantly more likely to develop eczema themselves.
Research from the American Academy of Paediatrics published in 2025 confirms that the condition involves a complex interplay between a defective skin barrier, immune dysfunction, and the skin’s microbiome. Consequently, managing eczema in children requires a holistic approach that addresses all of these factors rather than simply treating symptoms as they appear.
Recognising the Signs of Eczema in Children at Every Age
One of the most important things to understand about eczema in children is that it looks different at different ages. The location and appearance of the rash change as a child develops, which can sometimes make it difficult for parents to recognise. Below is a guide to what eczema in children typically looks like across different age groups.
Eczema in babies (0–12 months)
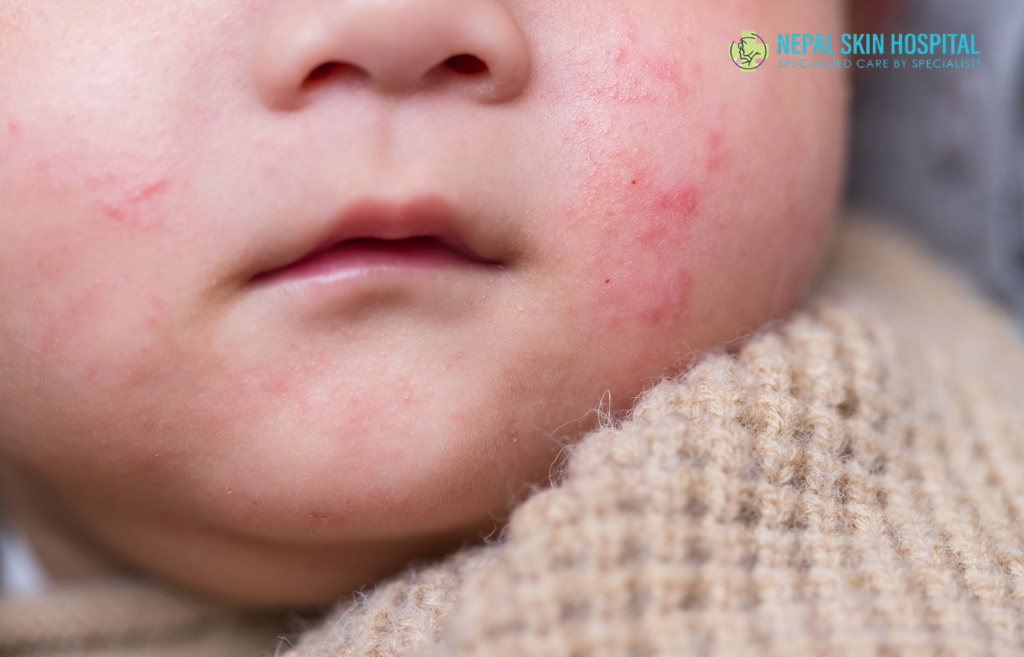
In infants, eczema most commonly appears first on the cheeks, forehead, and scalp. The rash typically presents as dry, red, and scaly patches that can weep or crust over when scratched. Babies with eczema are frequently irritable and restless, particularly at night, because the itching is especially intense during sleep hours. On darker skin tones, the rash may appear purple, grey, or brown rather than red, which is why eczema in children with darker complexions is sometimes missed or misdiagnosed.
Eczema in toddlers (1–5 years)
As a child moves into the toddler years, eczema in children tends to migrate from the face to the creases of the body, particularly inside the elbows, behind the knees, around the wrists, and on the ankles. The skin in these areas may become thickened and leathery from repeated scratching, a process known as lichenification. Toddlers with eczema often scratch instinctively and persistently, sometimes to the point of drawing blood, which significantly increases the risk of skin infection.
Eczema in school-aged children (6–12 years)
In older children, eczema typically continues to affect the same crease areas but may also appear on the hands, feet, eyelids, and neck. School-aged children with eczema face additional challenges: the visible rash, constant scratching, and disrupted sleep can affect concentration, school performance, and social confidence. Moreover, this age group is more susceptible to skin infections caused by bacteria such as Staphylococcus aureus, particularly when the skin barrier is repeatedly broken by scratching.
Key signs to look for in eczema in children at any age:
- Dry, itchy, red, or discoloured patches of skin
- Skin that weeps, crusts, or oozes, particularly after scratching
- Thickened or leathery patches in areas of repeated scratching
- Intense itching that worsens at night or after exposure to heat
- Recurring rashes in the same areas of the body
- Restless sleep and irritability due to discomfort
Common Triggers of Eczema in Children: What Parents Need to Know
Understanding what triggers eczema in children is one of the most powerful tools a parent can have. While eczema has no single cause, flare-ups are almost always precipitated by specific triggers that irritate the already-compromised skin barrier. Identifying and avoiding these triggers consistently is one of the most effective long-term strategies for managing eczema in children.
Environmental irritants
Certain substances in the environment directly irritate the skin of children with eczema, triggering inflammation even without an allergic reaction. The most common environmental irritants include:
- Soaps, bubble baths, shampoos, and cleansers containing fragrances or harsh sulfates
- Laundry detergents or fabric softeners with synthetic fragrances
- Rough or scratchy fabrics such as wool and synthetic fibres
- Cigarette smoke and air pollution`
- Excessive heat, sweating, and rapid temperature changes
- Dry or cold air, particularly common during Nepal’s winter months
Allergens
In addition to direct irritants, airborne and food allergens can trigger immune responses that worsen eczema in children. Common allergens include:
- House dust mites are one of the most frequent triggers of eczema in children
- Pet dander from cats and dogs
- Pollen, particularly during seasonal changes
- Mould spores in damp environments
- Food allergens, most commonly cow’s milk, eggs, peanuts, soy, and wheat, in younger children
However, it is important to note that food allergies are not the root cause of eczema in children. Furthermore, eliminating foods from a child’s diet without professional guidance can lead to nutritional deficiencies. Therefore, always consult a dermatologist or allergist before making significant dietary changes.
Skin infections
Children with eczema have a weakened skin barrier that makes them more vulnerable to bacterial, viral, and fungal infections. Staphylococcus aureus bacteria, in particular, colonise the skin of most children with eczema and can significantly worsen inflammation. When an infection is suspected, indicated by weeping, yellow crusting, increased swelling, or fever, it requires prompt medical attention rather than home management alone.
Stress and emotional factors
Finally, emotional stress is a well-recognised trigger for eczema in children. School pressures, anxiety, and major life changes can all provoke flare-ups by triggering the immune system’s inflammatory response. Consequently, supporting your child’s emotional well-being is an often-overlooked but genuinely important part of managing eczema in children.
Soothing Strategies for Eczema in Children: A Parent’s Practical Guide
While there is currently no cure for eczema in children, the condition can be very effectively managed with a consistent daily approach. The goal of management is two-fold: to prevent flare-ups from occurring and to provide immediate relief when they do. Below are the most evidence-backed soothing strategies recommended by dermatologists worldwide.
Strategy 1: Master the soak and seal method
Bathing is one of the most powerful tools in managing eczema in children, but only when done correctly. The recommended approach is known as the soak and seal method, which involves bathing the child in lukewarm water for 5 to 10 minutes, then immediately applying a thick moisturiser to damp skin within three minutes of leaving the bath to lock in the absorbed moisture.
Specifically, follow these guidelines for eczema-friendly bathing:
- Use lukewarm water only; hot water strips natural oils and worsens dryness.
- Keep baths short, 5 to 10 minutes maximum.
- Use a mild, fragrance-free, sulphate-free cleanser. Only apply cleanser to areas that truly need it.
- Avoid bubble baths, scented oils, and any product containing fragrance.
- After the bath, gently pat, never rub, the skin dry with a soft towel, leaving it slightly damp.
- Apply a thick, fragrance-free moisturiser or emollient immediately while the skin is still damp.
Strategy 2: Moisturise consistently — every single day
Moisturizing is the cornerstone of managing eczema in children, and it must be done consistently, not just during flare-ups. Apply a fragrance-free, hypoallergenic moisturizer or emollient to your child’s entire body at least twice daily, even when the skin looks clear. This daily habit repairs and reinforces the skin barrier over time, reducing both the frequency and severity of flare-ups.
In terms of formulation, thick creams and ointments are generally more effective than thin lotions for eczema in children, because they contain more oil and are better at sealing in moisture. Ingredients such as ceramides, hyaluronic acid, colloidal oatmeal, and glycerin are particularly beneficial for eczema-prone skin as they support barrier repair and provide soothing relief.
Strategy 3: Dress your child in skin-friendly fabrics
The clothing your child wears directly affects their skin throughout the day. For children with eczema, the best choice is soft, breathable, natural fabrics, particularly 100% cotton, bamboo, or silk. These materials allow the skin to breathe and minimize friction and irritation. Conversely, avoid wool, polyester, and nylon, which are known to aggravate eczema in children by causing friction and trapping heat.
Additionally, wash all new clothing before your child wears it for the first time, using a mild, fragrance-free laundry detergent. Avoid fabric softeners and dryer sheets, which often contain fragrance chemicals that can trigger flare-ups.
Strategy 4: Keep nails short and manage scratching
Scratching is one of the most damaging things a child with eczema can do to their skin. It breaks the skin barrier, worsens inflammation, spreads bacteria, and significantly increases the risk of infection and scarring. Nevertheless, telling a child to stop scratching is rarely effective on its own; the itch is genuinely intense and difficult to resist.
Instead, try these approaches:
- Keep your child’s nails trimmed short and smooth at all times.
- For babies and toddlers, use cotton mittens or eczema sleeves at night when scratching is most likely.
- Apply a cool, damp compress to intensely itchy areas for temporary relief; this soothes the itch without damaging the skin.
- Distract younger children from the itch with a favourite activity or toy.
- For older children, gently press or pat the itchy area rather than scratching it.
Strategy 5: Manage the home environment
Since dust mites are one of the most common triggers for eczema in children, reducing their presence in your home can make a meaningful difference. Furthermore, maintaining an optimal indoor environment generally supports skin health for eczema-prone children. Specifically:
- Wash bedding at 60°C or higher at least once a week to kill dust mites.
- Use dust-mite-proof covers on mattresses and pillows.
- Keep the home well-ventilated and avoid excessive humidity, which encourages mould growth.
- Use a humidifier in dry weather, particularly during Nepal’s dry winter months, to prevent the skin from losing moisture to the air.
- Vacuum regularly and minimise soft furnishings, rugs, and carpets where dust mites accumulate.
- If pets are a known trigger, limit their access to your child’s bedroom.
Strategy 6: Establish a calming bedtime routine
Eczema in children is almost universally worse at night. The combination of body heat under blankets, unconscious scratching during sleep, and reduced distraction makes nighttime particularly challenging. Therefore, a structured, calming bedtime routine can significantly reduce nighttime flare-ups and improve your child’s sleep quality.
After the evening bath and moisturising routine, dress your child in soft, breathable cotton pyjamas. Keep the bedroom cool and well-ventilated. For severe cases, wet wrap therapy, which involves applying a layer of prescribed treatment or moisturiser followed by damp and dry layers of soft fabric, can be very effective at reducing overnight itching when recommended by a dermatologist.
When Home Care Is Not Enough: Medical Treatment for Eczema in Children
While the soothing strategies above are highly effective for mild to moderate eczema in children, there are times when medical treatment is necessary. Specifically, consult a dermatologist if:
- Your child’s eczema is not improving despite consistent moisturising and trigger avoidance.
- The eczema is causing significant sleep disruption, school absence, or emotional distress.
- You notice signs of a skin infection, including weeping, yellow crusting, increased redness, swelling, or fever.
- Your child is scratching to the point of breaking the skin or bleeding.
- The eczema is severe, widespread, or involves sensitive areas such as the face, eyelids, or genitals.
Medical treatments for eczema in children range from topical corticosteroids and calcineurin inhibitors for mild to moderate cases, to biologic therapies such as dupilumab, approved for children aged 6 months and above, for severe, treatment-resistant eczema. Additionally, phototherapy is available for older children with widespread eczema that has not responded to other treatments. Our experienced dermatologists will assess your child’s individual needs and recommend the most appropriate, evidence-based treatment plan.
The Emotional Impact of Eczema in Children — and How to Support Your Child
It is important not to underestimate the emotional toll that eczema in children can take on the whole family. Research published in the journal Pediatrics confirms that the impact of eczema on quality of life is comparable to chronic conditions such as asthma and arthritis. Children with eczema frequently experience disrupted sleep, reduced concentration, lower self-esteem, and, in some cases, social withdrawal or depression.
As a parent, one of the most valuable things you can do is acknowledge your child’s discomfort without minimising it. Let your child know that eczema is not their fault and that many other children experience the same thing. Encourage open conversations about how the condition makes them feel. Furthermore, work with your child’s school to ensure teachers understand the condition and can provide support if needed.
Most importantly, remind your child and yourself that eczema in children is manageable. With the right care, the right triggers identified, and the right professional support in place, most children with eczema live full, comfortable, and active lives.
Frequently Asked Questions About Eczema in Children
Many children do improve significantly as they get older. Research shows that for many cases of eczema in children, symptoms begin to ease around the age of 5 to 6 years, and a significant proportion of children experience substantial improvement or complete remission by adolescence. However, some children continue to have eczema into adulthood, particularly if the condition is severe or if asthma and allergies are also present. Therefore, ongoing management and regular dermatological review remain important.
Food allergies can trigger eczema flare-ups in some children, particularly in infants and toddlers, but they are not the underlying cause of eczema. The most common food triggers include cow’s milk, eggs, peanuts, soy, and wheat. However, it is essential not to eliminate foods from your child’s diet without professional guidance, as unnecessary dietary restriction can impact growth and nutrition. An allergist can conduct appropriate testing to determine whether specific food allergies are contributing to your child’s eczema.
Yes, Because eczema weakens the skin barrier, children with eczema are significantly more vulnerable to skin infections, particularly from Staphylococcus aureus bacteria. Signs of infection include increased weeping, yellow or honey-coloured crusting, swelling, warmth, and fever. If you suspect your child’s eczema has become infected, seek medical attention promptly, as infections require antibiotic treatment and can worsen eczema significantly if left untreated.
Final Thoughts: You Are Not Alone in Managing Eczema in Children
Eczema in children can feel relentless at times, particularly during severe flare-ups or periods of disrupted sleep. Nevertheless, it is important to remember that you are not alone and that this condition is entirely manageable with the right approach.
To summarise: eczema in children is a chronic but treatable inflammatory skin condition caused by a combination of genetic factors, a weakened skin barrier, and environmental triggers. The most effective management combines consistent moisturising, the soak and seal bathing method, trigger identification and avoidance, appropriate clothing choices, and, when needed, professional medical treatment.
If you are concerned about your child’s skin, do not hesitate to book an appointment with our team at Nepal Skin Hospital. We offer comprehensive assessment and personalised care for eczema and all skin conditions in children of all ages. Because every child deserves comfortable, healthy skin, and every parent deserves the confidence that comes from knowing exactly what to do.









