
Acne is one of the most common skin conditions in the world, and yet it remains one of the most misunderstood. Many people assume that knowing how to treat acne is straightforward: wash your face, avoid greasy food, and wait it out. However, the reality is far more nuanced. Acne can affect people of all ages, from teenagers going through puberty to adults in their 40s and 50s who have never had a breakout before. It can range from a few occasional pimples to deep, painful cysts that leave permanent scars.
According to the American Academy of Dermatology, acne affects up to 50 million people every year, making it the most prevalent skin condition globally. Furthermore, research shows that approximately 85% of teenagers experience acne, while up to 50% of women and 25% of men in their 20s and 30s continue to struggle with adult breakouts. In some cases, acne can even persist into the 40s and 50s, or appear for the very first time in adulthood.
Therefore, understanding what causes acne at different stages of life, what triggers flare-ups, and, most importantly, how to treat it effectively is essential for anyone dealing with this condition. If breakouts are affecting your confidence or daily life, our qualified skin specialists are here to help you find the right solution.
What Is Acne and How Does It Form? (And How to Treat It)
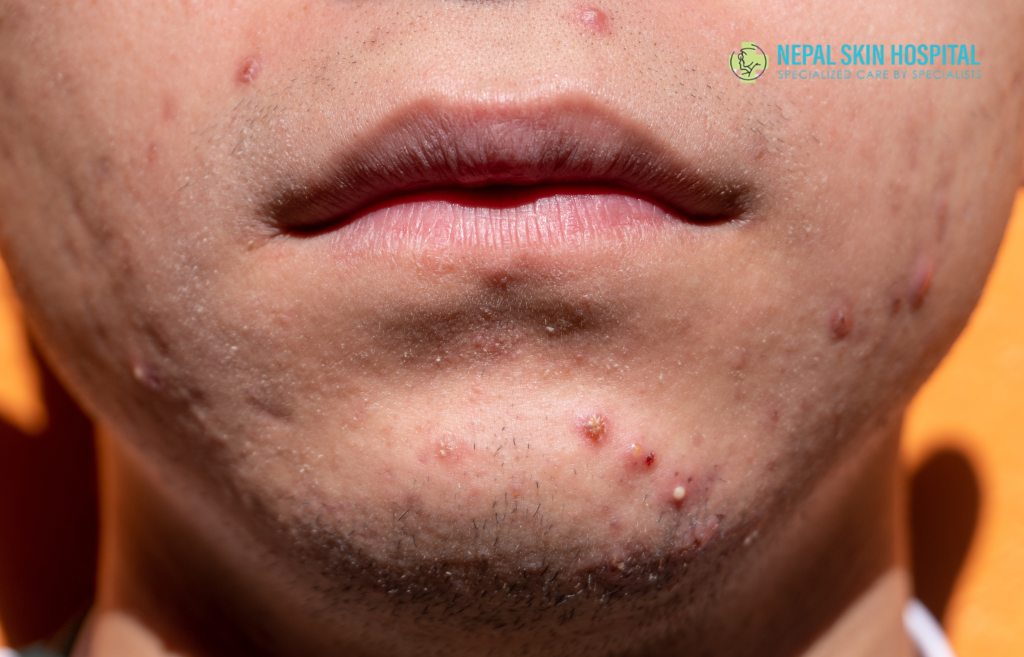
Before exploring how to treat acne, it is helpful to understand exactly what it is and how it develops. Acne occurs when hair follicles, the tiny pores on the surface of your skin, become blocked with a combination of excess oil (called sebum), dead skin cells, and bacteria. This blockage creates an ideal environment for a specific type of bacteria called Cutibacterium acnes (formerly Propionibacterium acnes) to multiply, triggering inflammation and the formation of various types of lesions.
Depending on how the blockage occurs and the level of inflammation, acne can take several forms:
- Whiteheads: Closed, blocked pores with trapped oil and dead skin cells beneath the skin’s surface.
- Blackheads: Open, clogged pores where the trapped material is exposed to air, causing oxidation and a dark appearance.
- Papules: Small, raised, red bumps caused by inflammation around the follicle.
- Pustules: Inflamed papules with a visible white or yellow centre containing pus.
- Nodules: Large, solid, painful lumps deep within the skin, a sign of more severe acne.
- Cystic acne: The most severe form, involving large, pus-filled cysts deep beneath the skin that carry a high risk of scarring.
Consequently, not all acne is the same. As a result, treatment needs to be tailored to the type and severity of the breakout, as well as to the age and hormonal profile of the individual.
Why Does Acne Happen? The Root Causes
Acne is a multifactorial condition, meaning it is caused by a combination of factors rather than a single trigger. Nevertheless, four core mechanisms are consistently identified in dermatological research:
1. Excess sebum production
Sebum is the natural oil produced by the skin’s sebaceous glands to keep skin moisturised and protected. However, when these glands produce too much sebum, often triggered by hormonal activity, the excess oil mixes with dead skin cells and clogs pores. This overproduction is the primary driver of most acne, which is why hormonal changes are so closely linked to breakouts.
2. Abnormal skin cell shedding
Under normal circumstances, the skin continuously sheds dead cells to renew itself. However, in acne-prone individuals, dead skin cells shed too quickly and stick together inside the hair follicle rather than being expelled naturally. As a result, they form a plug that traps sebum and creates the ideal environment for bacterial growth.
3. Bacterial colonisation
While Cutibacterium acnes is naturally present on everyone’s skin, it thrives in the oxygen-deprived environment of a blocked pore. As it multiplies, it triggers an immune response, causing the redness, swelling, and pus associated with inflammatory acne. Notably, however, the presence of bacteria alone does not cause acne, it is the combination of excess sebum, blocked pores, and bacterial overgrowth that creates the problem.
4. Inflammation
Inflammation is the body’s natural response to infection and injury. In acne, however, it is the inflammatory response that causes the most visible and lasting damage. When the immune system attacks the bacteria inside a blocked pore, the surrounding tissue becomes red, swollen, and painful. In more severe cases, this inflammation can extend deep into the skin, increasing the risk of permanent scarring.
Acne at Every Age: How It Differs and Why

Acne in children (under 9 years)
Although relatively uncommon, acne can occur even in newborns and young children. Neonatal acne, which affects approximately 20% of newborns, typically appears within the first six weeks of life and is usually mild and self-limiting, resolving without treatment. Similarly, infantile acne may develop between six weeks and one year of age and is more common in boys.
However, if acne appears in children between the ages of 1 and 7, a stage known as mid-childhood acne, it is generally considered a sign of an underlying hormonal imbalance and warrants medical evaluation by a specialist.
Teenage acne (ages 9–19)
Teenage acne is the most widely recognised form, and for good reason. During puberty, the body produces a surge of hormones known as androgens, including testosterone in boys and progesterone in girls. These androgens stimulate the sebaceous glands to produce significantly more sebum than usual, setting the stage for breakouts.
Consequently, teenage acne tends to appear in the T-zone, the forehead, nose, and chin, as well as on the chest and back, where oil glands are particularly active. While teenage acne is an entirely normal part of development, it can have a profound impact on self-esteem. Therefore, understanding how to treat acne during adolescence is especially important, as untreated breakouts carry a significant risk of scarring that can persist into adulthood.
Adult acne (ages 20–39)
One of the most important things to understand about adult acne is that it is far more common than many people realise. In fact, research published in the Journal of Women’s Health found that up to 50% of women in their 20s and 30s experience acne. Meanwhile, adult acne in men, though less common, is also widely reported.
Unlike teenage acne, adult acne is more likely to appear on the lower face, particularly along the jawline, chin, and neck. This distribution is characteristic of hormonal acne and is strongly associated with fluctuations in oestrogen and progesterone. Common triggers in adults include:
- Hormonal changes related to the menstrual cycle, pregnancy, or conditions such as polycystic ovary syndrome (PCOS).
- Chronic stress, which causes the body to release cortisol, a hormone that increases sebum production and inflammation.
- A high-glycaemic diet high in refined sugars, processed foods, and dairy, which raises insulin levels and stimulates oil production.
- Comedogenic skincare or cosmetic products that block pores.
- Certain medications, including steroids, lithium, and some contraceptives.
- Genetics, a strong family history of adult acne, significantly increases the risk.
Moreover, adult skin heals more slowly than teenage skin. As a result, adult acne breakouts tend to be deeper, more inflammatory, and more likely to leave lasting marks. This makes early treatment particularly critical for this age group.
Acne in adults over 40
While it may come as a surprise, acne can continue, or even begin for the first time, in people over 40. For women, this is often linked to the hormonal shifts of perimenopause and menopause, during which fluctuating oestrogen and progesterone levels can destabilise sebum production and trigger breakouts. For men, late-onset acne is less common but can be associated with hormonal changes, stress, or the use of certain supplements and medications.
In either case, treating acne in this age group requires a particularly thoughtful approach, since older skin tends to be drier, thinner, and more sensitive than younger skin. Consequently, aggressive treatments that might work well for teenagers can cause irritation, dryness, and increased sensitivity in mature skin.
How to Treat Acne: Evidence-Based Approaches

The good news is that, regardless of age, acne can be effectively managed with the right approach. The key, however, is understanding that no single treatment works for everyone. Instead, effective acne management typically involves a combination of skincare habits, lifestyle adjustments, and in moderate to severe cases, professional treatment.
Daily skincare habits
First and foremost, a consistent and gentle daily skincare routine is the foundation of any acne management plan. Specifically, this should include:
- Washing the face twice daily with a mild, non-comedogenic cleanser to remove excess oil, sweat, and impurities without stripping the skin.
- Avoid harsh scrubs, rough cloths, or vigorous rubbing, all of which can irritate acne-prone skin and worsen inflammation.
- Using a lightweight, oil-free moisturiser to maintain the skin’s barrier function without adding excess oil.
- Never pick, squeeze, or press on acne lesions; doing so introduces additional bacteria, worsens inflammation, and significantly increases the risk of permanent scarring.
- Removing makeup thoroughly before bed and only using non-comedogenic cosmetic products.
Diet and lifestyle adjustments
In addition to skincare, diet and lifestyle play a meaningful role in acne management. Although food alone does not cause acne, research consistently shows that certain dietary patterns can worsen breakouts in predisposed individuals. In particular:
- A high-glycaemic diet, rich in white bread, sugary drinks, refined carbohydrates, and processed snacks, raises blood insulin levels, which in turn stimulates androgen activity and increases sebum production.
- Dairy products, particularly milk, have also been associated with acne flare-ups in some individuals, possibly due to hormones present in cow’s milk.
- Conversely, an anti-inflammatory diet rich in omega-3 fatty acids (found in oily fish, walnuts, and flaxseeds), antioxidants (from colourful fruits and vegetables), and low-glycaemic foods appears to support clearer skin.
Furthermore, managing stress is critically important for acne-prone individuals. This is because stress triggers the release of cortisol, which stimulates the sebaceous glands and increases inflammatory responses in the skin. Regular exercise, adequate sleep, and relaxation techniques such as meditation or yoga can all help regulate cortisol levels and reduce stress-related breakouts.
Professional treatments for acne
For moderate to severe acne, or for acne that does not respond to home care, professional dermatological treatment is highly effective. In fact, seeking professional care early is one of the most important steps you can take to prevent permanent scarring. Depending on the severity and type of acne, a dermatologist may recommend:
- Topical retinoids: Derived from vitamin A, retinoids promote cell turnover, prevent pore blockages, and reduce inflammation. They are among the most evidence-backed topical treatments available for acne.
- Topical or oral antibiotics: These reduce the population of Cutibacterium acnes on the skin. Oral antibiotics such as doxycycline are particularly effective for inflammatory acne.
- Hormonal therapies: For women with hormonal acne, treatments that regulate androgen levels can significantly reduce breakouts.
- Chemical peeling: This treatment removes damaged outer layers of skin, unclogs pores, and stimulates the regeneration of smoother, clearer skin. It is particularly effective for acne and post-acne hyperpigmentation.
- Laser and light therapies: These target the bacteria responsible for acne and reduce inflammation. They can also improve the appearance of acne scars.
- Isotretinoin: A powerful oral retinoid reserved for severe or treatment-resistant cystic acne. When prescribed and monitored by a dermatologist, it remains one of the most effective acne treatments available.
At Nepal Skin Hospital, our experienced dermatologists offer a full range of professional acne treatments tailored to your skin type and age. In particular, our chemical peeling treatments have helped many patients achieve significantly clearer skin. Additionally, we offer advanced laser and cosmetic treatments for both active acne and acne scarring.
How to Prevent Acne Scarring
Acne scars are one of the most distressing consequences of severe or poorly managed breakouts. Fortunately, however, there are concrete steps you can take to minimise the risk of scarring:
- Treat acne early; do not wait until breakouts become severe. Early intervention reduces inflammation and the likelihood of deep tissue damage.
- Never pick or squeeze lesions; this is the single most common cause of permanent acne scarring.
- Use a broad-spectrum sunscreen daily, as sun exposure darkens post-acne marks and makes them significantly more visible and longer-lasting.
- Follow your dermatologist’s treatment plan consistently; incomplete treatment allows acne to return and worsen over time.
If you already have acne scars, several effective treatments are available, including chemical peeling, laser resurfacing, microneedling, and dermal fillers. The most appropriate option depends on the type and depth of your scarring, which is why a consultation with a qualified dermatologist is the recommended first step.
When Should You See a Doctor About How to Treat Acne?

While mild acne can often be managed with good skincare habits and lifestyle changes, there are clear situations where professional medical care is not just helpful, it is essential. Specifically, you should consult a dermatologist if:
- Your acne is moderate to severe, covering large areas of the face, chest, or back.
- You have painful nodules or cysts beneath the skin.
- Your acne is not improving after six to eight weeks of consistent home care.
- You are developing dark marks or scars from previous breakouts.
- Your acne is affecting your confidence, mental health, or daily functioning.
- You are an adult experiencing new or worsening acne for the first time.
In any of these situations, do not delay seeking help. The earlier acne is treated professionally, the better the outcomes, and the lower the risk of permanent skin damage. You can easily book an appointment with our team at Nepal Skin Hospital to receive a personalised assessment and treatment plan.
Final Thoughts on How to Treat Acne at Every Age
Acne is not a condition limited to teenagers, nor is it something you simply have to live with. Regardless of your age, understanding how to treat acne effectively and acting on that understanding consistently can make a profound difference to the clarity and health of your skin.
To summarise: acne is caused by a combination of excess oil, blocked pores, bacterial growth, and inflammation. It affects people differently at every stage of life, and treatment must therefore be adapted to age, skin type, and the underlying causes of each individual’s breakouts. While home care and lifestyle changes are a valuable first step, moderate to severe acne almost always benefits from professional guidance.
If you are ready to take control of your acne, our dedicated team at Nepal Skin Hospital is here to help. From an initial skin assessment to advanced in-clinic treatments, we provide comprehensive, compassionate care for acne at every age. Because clear, healthy skin is not a luxury, it is something everyone deserves.









